(Courtesy of SMGH) It is a well-known fact that Ashkenazi Jews carry at least one of 38 genetic diseases, some of which include the BRCA 1 and 2 genes (cancer), Gaucher, Crohn’s disease and irritable bowel syndrome (IBS), among others. Today we would like to focus on these issues and how we treat them at St. Mary’s General Hospital in our newly constructed and renovated Endoscopy Center in contemplation of a webinar we are planning for January 21.
The Endoscopy Center at St. Mary’s General Hospital performs upper and lower gastrointestinal procedures such as colonoscopies, endoscopies, gastroscopies, esophagogastroduodenoscopies1 (EGDs), endoscopic retrograde cholangiopancreatographies2 (ERCPs) and percutaneous endoscopic gastrostomy3 (PEG) insertions. The unit services outpatients with two fully-staffed procedure rooms, all in a warm and pleasant environment geared at making patients feel comfortable and at ease throughout their experience. The Endoscopy Center is staffed with North Jersey’s leading certified specialists in gastroenterology, some of whom we will be featuring soon.
“St. Mary’s General Hospital has a long history with oncology and treating cancer patients,” said George Matyjewicz, PhD, community liaison, “dating back to the original Passaic Beth Israel Hospital (PBI), which was funded by the local Jewish community and was a leader in treating cancer, with a respected center of excellence in oncology. Today, as part of the $65 million Prime Healthcare improvements the department has been expanded and upgraded to include new state-of-the-art equipment and top physicians to treat patients.”
Why do I need an endoscopic procedure? Maybe that stomach pain is not from what you ate today—maybe it’s something more serious. Endoscopy is the examination of the inside of the body (commonly the esophagus, stomach and portions of the intestine) by using a lighted, flexible instrument called an endoscope. Abdominal tests are performed to diagnose colitis; colon, stomach or pancreatic cancer; gallstones; and ulcers.
Modern advances in technology have greatly improved the accuracy, speed and ease of establishing the cause of abdominal pain, but significant challenges remain, especially when symptoms don’t fit a textbook diagnosis. A patient may be taking medications, vitamins, minerals or food supplements that reduce inflammation and they have little pain. Crohn’s disease can mimic appendicitis. IBS symptoms can mimic bowel obstruction, cancer, ulcer, gallbladder attacks or even appendicitis. A ruptured right ovarian cyst can mimic appendicitis, while a ruptured left ovarian cyst can mimic diverticulitis. Or the characteristics of the pain may change.
An endoscopic procedure will help eliminate misdiagnosed illnesses and help you treat these issues.
Then what happens? Once the results of the endoscopic procedure have been reviewed and analyzed, a treatment plan can be ordered to help you get better more quickly. There are a number of treatments that may include medication, diet or even surgery. Most importantly your pain and suffering will go away more quickly now that you have been accurately diagnosed.
Keep in mind that a procedure like colonoscopy should be done by age 50 or sooner if you have a family history of bowel cancer, or if you have any previously diagnosed conditions that affect your digestive tract, including irritable bowel syndrome (IBS), inflammatory bowel disease (IBD) or colorectal polyps. Also, as you age, your risk of developing polyps and bowel cancer increases. Getting routine colonoscopies helps your doctor find abnormalities early so they can be quickly treated.
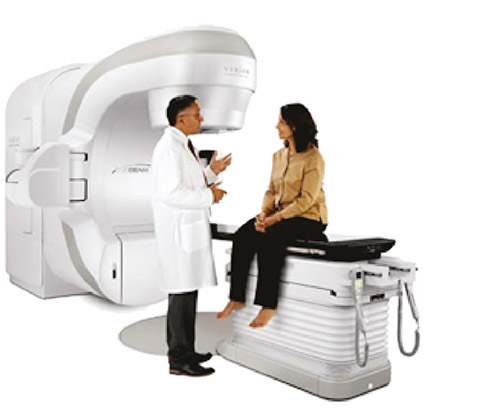
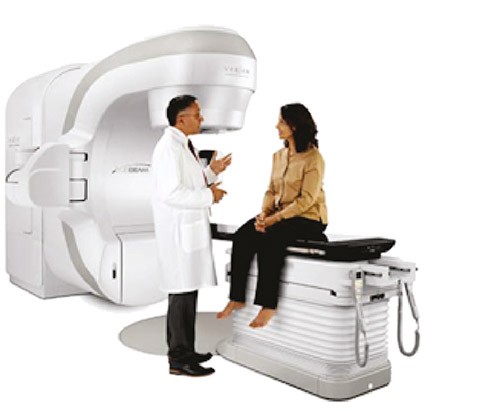
Will I need surgery? Whether or not you need surgery will depend on the results of your testing. Medicine has come a long way since the days of blood letting, and surgeries are not what your parents experienced even at the turn of this century. With today’s technology, surgeries are often same-day and use robots for more accuracy and for smaller scars. For example, at St. Mary’s General we have a multi-million dollar TrueBeam® Radiotherapy System for cancer patients, which minimizes damage to surrounding tissue, and in some cases treatment takes fewer than five visits!
With good diagnostic and screening technologies, our experts are able to diagnose your condition in its earliest stages. With equipment like the TrueBeam® Radiotherapy System, our clinical team, lead by an expert radiation oncologist, is able to treat your cancer without surgery, using powerful, state-of-the-art radiotherapy individualized for your condition. This is non-invasive treatment—no incisions or surgery. Your physician can use radiotherapy or radiosurgery, whichever is appropriate for your specific cancer. You can be in and out of the cancer center in 20 minutes!
We provide many other radiation-therapy options, including the most advanced procedures and treatment technology available—RapidArc® volumetric arc therapy, intensity-modulated radiation therapy (IMRT) and image-guided therapy (IGRT). And most important is the diagnosis as determined by the professional staff in the Endoscopy Center!
St. Mary’s General Hospital—nationally recognized, locally preferred among the top hospitals in America for health, quality and patient safety! The hospital has over 550 physicians and 1,200 employees, with every staff member committed to providing respectful, personalized, high-quality care—to satisfy patients’ needs and exceed their expectations. St. Mary’s General is a proud member of Prime Healthcare, which has more Patient Safety Excellence Awards for five consecutive years (2016-2020) than any other health system in the country, including a “Top 15 Healthcare System” by Truven Health Analytics. To learn more about St. Mary’s General Hospital visit https://www.smh-nj.com/ or Facebook at https://www.facebook.com/StMarysGeneral.
For more information, please contact George Matyjewicz, PhD, community liaison at [email protected].
1 EGD is a procedure that examines the esophagus, stomach and first portion of the small intestine (the duodenum) using a long flexible tube with a camera at the end of it. The scope is inserted into the mouth and advanced to the small intestine.
2 ERCP is a procedure used to diagnose diseases of the gallbladder, biliary system, pancreas and liver. The test looks “upstream” where digestive fluid comes from—the liver, gallbladder and pancreas—to where it enters the intestines.
3 PEG is a procedure in which a flexible feeding tube is placed through the abdominal wall and into the stomach. PEG allows nutrition, fluids and/or medications to be put directly into the stomach, bypassing the mouth and esophagus.