We don’t have direct control over many aspects of the COVID-19 pandemic; however, if you are recovering from COVID-19, there is a great deal that can be done to change the trajectory of your recovery. While there currently is no known cure for COVID-19, there are empirically-based methods you can use to reduce the chances of secondary complications and hasten the return to your prior health.
The primary sequence of the COVID-19 attack on your body involves creating hemodynamic instability, which disrupts the production of Surfactant––a substance that allows gas exchange to occur in the lungs––leading to shortness of breath and an overwhelming immune response (“the cytokine storm”). There are also longer-term deficits that you must contend with, including extreme deconditioning, impaired endurance, impaired balance, muscle weakness, back, neck and shoulder stiffness and pain, headaches and the inevitable emotional impact of it all.
These potential long-term effects must be addressed if you wish to return back to your previous level of functioning. While the sequelae of events stemming from COVID-19 may be overwhelming, there is hope to be found in some simple guidelines. These are not in place of any official medical advice and your doctor or physical therapist should be consulted to tailor and monitor an individualized program that uniquely addresses your situation.
If you are recovering from COVID-19 you might feel extremely fatigued and weak. Just sitting upright may cause you to lose your breath. Whatever your level is, be sure to challenge yourself as much as you can tolerate, with another person or a phone nearby for safety. Staying in bed and remaining inactive can lead to skin breakdown and ulcers, and make you more susceptible to complications from blood clots. It can also contribute to depression and feelings of helplessness, which may not have been a factor in your life prior to being diagnosed with COVID-19. Begin a walking program that gradually increases from five minutes five times per day to 15 minutes twice per day to improve your overall conditioning.
For the first six to eight weeks of recovery, focus on low to moderate intensity exercise, with a goal of being able to perform your normal activities of daily living without difficulty. Be deliberate, set goals and chart out specific activities that will allow you to achieve those goals. After about 16 weeks, a higher level of activity can be resumed.
If you are recovering from a severe illness following prolonged hospitalization expect to see a rapid rise in heart rate, poor exercise tolerance, quick fatigue and low maximal performance. Keep an eye on blood pressure and oxygen saturation (measured with a pulse oximeter) and get guidelines from your doctor or physical therapist as to when exercise should be stopped.
Remember that being stationary for prolonged periods of time causes the body to stiffen. Most importantly, the rib cage has not been expanding fully to accommodate normal breathing, while the chest simultaneously stiffens and pulls you forward into a “slouched” posture. Some easy stretches to consider:
1) Doorway Pec Stretch: Stand in the middle of a doorway with one foot in front of the other. Bend your elbows at a 90-degree angle and place your forearms on each side of the doorway. Shift your weight onto your font leg and lean forward until you feel a stretch in your chest.
2) Sidebending stretch: While standing or sitting with your arms at your sides, reach down with one hand and bring your other arm over your head until you feel a stretch in your side.
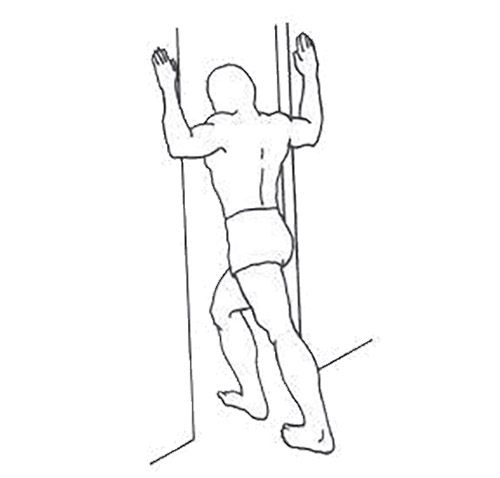
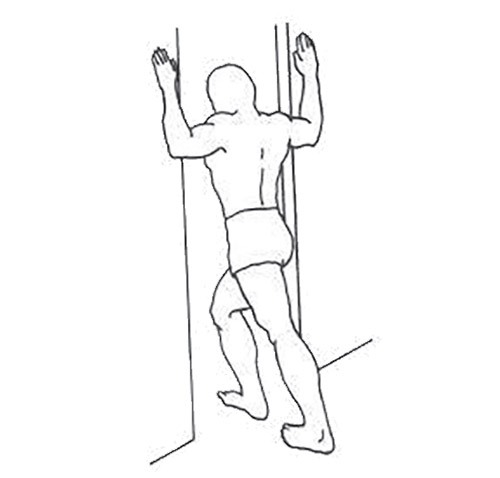
3) Wall Wash: Stand facing the wall and slide your hands straight up the wall as high as possible until you feel a stretch in the shoulders and upper back.
Each stretch can be held for 15 to 30 seconds and can be repeated three times.
Breathing exercises are critical when recovering from COVID-19. Some breathing exercises to consider:
1) Incentive Spirometer: (For those that were hospitalized have received an incentive spirometer upon discharge.) Make sure you are following the instructions as many people use this incorrectly. Use for 15 minutes throughout the day, which can be broken up into three sessions.
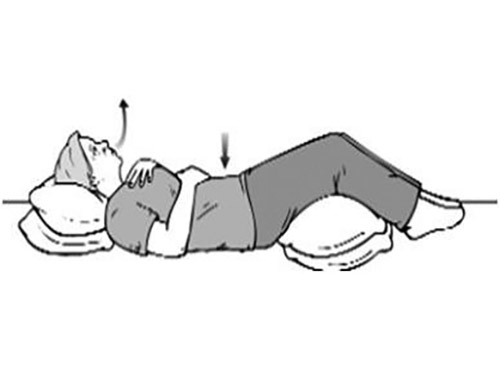
2) Diaphragmatic Breathing: While lying facing upward with your head on a pillow or sitting comfortably in a chair, put one hand on your belly and one on your chest. Breathe deeply through your nose, allowing your belly to expand, then slowly breathe out. This can be performed for one minute.
3) Place a paper or plastic cup face-down on a table or counter in front of you. Blow through a straw and attempt to push the cup along the table. Blow for three to five seconds, 10 to 15 times per hour or as tolerated.
If you are currently recovering from COVID-19, your body has been through quite a bit. It will take some time to return to your baseline, but the overwhelming majority of you will get there. Be an active participant in your recovery and take the steps necessary to ensure you recover fully and as fast as possible while minimizing any potential complications along the way. Stay in close contact with your doctor and work with a physical therapist so you can be confident you are safe and heading in a positive direction. Keep a strong support system and don’t underestimate the power of laughter and positivity, both of which are strong healing tools that help make everything more manageable and efficacious.
Aharon Bauman PT, DPT, is an orthopedic physical therapist licensed in NY and NJ. Aharon currently works at Mount Sinai Union Square in Manhattan. During the COVID-19 pandemic he has been treating patients with COVID-19 at Mount Sinai Beth Israel hospital in Manhattan. Aharon also treats patients privately in Northern N.J., or via telehealth. He can be reached at [email protected]